What does the procedure involve?
Removal of a small section of vas from both sides with insertion of tissue between the divided ends to prevent re-joining.
What are the alternatives to this procedure?
Alternatives to this procedure include other forms of contraception (both male and female).
Vasectomy should be regarded as an “irreversible” procedure. If you have any doubt about whether it is the right option for you, you should not go ahead with the operation. Under normal circumstances, vasectomy is not appropriate during pregnancy or within the first six months after the birth of a child.
What should I expect before the procedure?
Vasectomy is usually a day surgery procedure that can be performed under local or general anaesthetic.
Please inform your surgeon (before your surgery) if you have any of the following:
- An artificial heart valve.
- A coronary artery stent.
- A heart pacemaker or defibrillator.
- An artificial joint.
- An artificial blood-vessel graft.
- A neurosurgical shunt.
- Any other implanted foreign body.
- A regular prescription for a blood thinner e.g. Warfarin, Coumadin Xarelto®, Pradaxa®, Clopidogrel (Plavix®), Brilinta®, or Aspirin.
- Previous or current infection with an antibiotic resistant organism such as MRSA, VRE, etc.
What happens during the procedure?
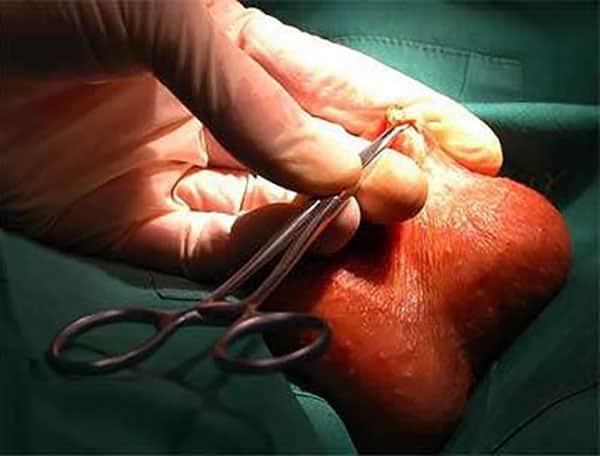
Vasectomy can be performed under a local or general anaesthetic according you your preference. If your tubes are difficult to feel, however, vasectomy may need to be done under a brief general anaesthetic.
When a local anaesthetic is used it is uncomfortable when you have the local anaesthetic injected but it numbs the skin quickly. However, local anaesthetic may not make the procedure completely painless; the act of picking up the tubes (pictured) can cause a variable degree of discomfort. This may make you feel slightly sick, sweaty or light-headed.
What happens immediately after the procedure?
It is essential to have someone to drive you home after the procedure; you should not attempt to drive yourself. We advise you to take the next day off work and sit quietly at home. The local anaesthetic will wear off after a couple of hours and the area may ache for 24 to 72 hours. You can usually relieve this by taking paracetamol.
Are there any side-effects?
Although the complications listed below are well recognised, most patients do not suffer any problems.
Common (greater than 1 in 10)
- A small amount of bruising and scrotal swelling for several days.
- Seepage of a small amount of clear, yellow fluid several days later.
- Blood in the semen for the first few ejaculations.
- The procedure should be regarded as irreversible. Although vasectomy may be reversed, this is not always effective in restoring fertility, especially if more than 7 years have lapsed since the vasectomy.
- Contraception must be continued after vasectomy until no motile sperms are present in two consecutive semen samples.
- Chronic testicular pain (10 %) or sperm granuloma (tender nodule at the site of surgery).
Occasional (between 1 in 10 and 1 in 50)
- Significant bleeding or bruising needing further surgery.
- Inflammation or infection of the testes or epididymis needing antibiotic treatment.
Rare (less than 1 in 50)
- Early failure of the procedure to produce sterility (1 in 250 to 500).
- Re-joining of vas ends, after negative sperm counts, resulting in fertility and pregnancy at a later stage (1 in 2000).
When you leave hospital
Over the first few days, your scrotum and groins may become a little uncomfortable and bruised. It is not unusual for the wound to appear swollen and slightly weepy; if you are worried about this, you should contact your GP or Dr Nathan’s rooms. Your sutures do not need to be removed and will usually drop out after a couple of weeks although, sometimes, they may take slightly longer.
What else should I look out for?
If you develop a temperature, increased redness, throbbing or drainage at the site of the operation, please contact Dr Nathan’s rooms or your GP.
Are there any other important points?
Many people ask if they are “too young” to have a vasectomy. There are no rules about how old you should be and each individual case will be considered on its own merits. However, vasectomy is not an appropriate form of contraception for a single man unless there are specified (and rare) medical conditions such as a severe inherited disease.
You are not sterile immediately after the operation.
This is because some sperms have already passed beyond the site where the tubes are tied off. These sperms are cleared by normal ejaculation. On average, you will need 20 to 30 ejaculations to clear these sperms. 3 months after the operation, you will be asked to produce specimens of semen for examination under a microscope. Please read the instructions for production and delivery of these specimens very carefully. If no sperms are present, you are sterile. If there are still a few non-motile or dead sperms, you may be regarded as sterile. If there are large numbers of motile sperms, you will need to provide further specimens until you are clear. Until you get the “all clear” you must continue with your contraceptive precautions.
Disclaimer
This information is intended as a general educational guide and may not apply to your situation. You must not rely on this information as an alternative to consultation with your urologist or other health professional.
Not all potential complications are listed, and you must talk to your urologist about the complications specific to your situation.
