What does the procedure involve?
This involves injecting Botox (Botulinium Toxin) into the wall of the bladder using a telescope inserted through the urethra (water-pipe), to overcome the effects of an overactive bladder.
Who is suitable for Botox?
Patients with a diagnosis of overactive bladder who suffer from a strong urge to pass urine (associated with urinary incontinence) that does not respond to medication. Botox injections may produce good symptom relief.
Additionally, patients with neurological problems causing an overactive bladder and / or high pressure in the bladder. Neurological conditions that affect the bladder include:
- Spinal Cord problems.
- Stroke.
- Multiple Sclerosis.
- Parkinson’s disease.
It is a well-tolerated procedure, but the effect is temporary, and injection may need to be repeated after approx. 9 months.
Men or women with the symptoms or problems mentioned above may be suitable for Botox injection into the bladder. Generally, patients should have gone through a series of other treatments such as bladder physiotherapy and / or bladder retraining, have tried oral medication for their symptoms, and have failed these treatments before Botox is considered.
What are the alternatives to this procedure?
Alternatives to this procedure include drug treatment, bladder training, physiotherapy, sacral nerve stimulation, bladder enlargement with a segment of bowel and urinary diversion into a stoma.
What should I expect before the procedure?
You will usually be admitted on the day of your surgery.
Please tell your surgeon (before your surgery) if you have any of the following:
- An artificial heart valve.
- A coronary artery stent.
- A heart pacemaker or defibrillator.
- An artificial joint.
- An artificial blood-vessel graft.
- A neurosurgical shunt.
- Any other implanted foreign body.
- A regular prescription for a blood thinner e.g. Warfarin, Coumadin Xarelto®, Pradaxa®, Clopidogrel (Plavix®), Brilinta®, or Aspirin.
- Previous or current infection with an antibiotic resistant organism such as MRSA, VRE, etc.
What happens during the procedure?
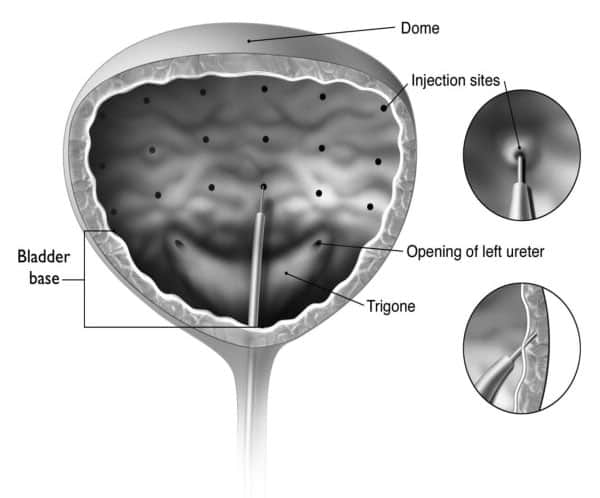
The procedure is usually performed under a general anaesthetic. The botulinum toxin is injected through a cystoscope (a telescope passed into the bladder via the water pipe.
What happens immediately after the procedure?
You may experience some discomfort for a few days after the procedure and you are usually given painkillers to take home.
The procedure is done on a day-case basis with a length of stay less than one day.
Are there any side-effects?
Most procedures have possible side-effects. But, although the complications listed below are well-recognised, most patients do not suffer any problems.
Common (greater than 1 in 10)
- Blood in the urine.
- Discomfort when passing urine.
- Urinary tract infection.
Occasional (between 1 in 10 and 1 in 50)
- Difficulty in emptying the bladder adequately, requiring the use of intermittent self-catheterisation (5-10%).
- Risk of recurrent urinary infections.>
Rare (less than 1 in 50)
- Generalised weakness due to the effect of the toxin on the muscles of the body, requiring admission to hospital.
What should I expect when I get home?
It is likely that you will see some blood in your urine and there will be slight discomfort while passing urine.
What else should I look out for?
If you develop difficulty emptying your bladder, please contact your Surgeon or Urology Nurse. The original symptoms may return after about nine months, requiring re-treatment.
Are there any other important points?
Because Botox inhibits the action of bladder muscle, it is possible that the effect may be too much for your bladder, and that you may not be able to pass urine normally for as long as it takes the effect of Botox to wear off (this can be as long as 9 months). This is rare, but if it occurred, you would need to perform intermittent self-catheterisation (ISC) (see ISC for males / ISC for females) for this period of time. It is usual for you to be taught ISC before you have Botox to ensure that, in the rare event that you were affected in this way, you would be able pass a catheter yourself.
Disclaimer
This information is intended as a general educational guide and may not apply to your situation. You must not rely on this information as an alternative to consultation with your urologist or other health professional.
Not all potential complications are listed, and you must talk to your urologist about the complications specific to your situation.
